Are you normal? How about your body temperature, blood pressure, blood glucose?
Body Temperature
Have you ever wondered how 98.6° Fahrenheit or 37° Centigrade became “normal” body temperature? In the 1850’s, a German physician named Carl Wunderlich collected data on 25,000 patients, taking their temperature multiple times. Wunderlich was the first to show how the body temperature fluctuates naturally throughout the day and night, and he was the first to set the threshold for fever (any temperature above 100.4 F).
fluctuates naturally throughout the day and night, and he was the first to set the threshold for fever (any temperature above 100.4 F).
But Wunderlich’s scientific method challenged one very contemporary creative thinker. Philip Mackowiak, a medical doctor, practicing in internal medicine and professor of medicine and medical historian at the University of Maryland, was intrigued by clinical thermometry, or the measurement of body temperature. He was able of obtain one of Wunderlich’s original thermometers.
To make a fun story short (and you can listen to the entire podcast on Freakonomics here), it turns out that Wunderlich only measured armpit (axillary) temperatures — today we know that the most accurate measurements are by mouth, or even better, rectally. The thermometer was unwieldy and most importantly, it was non-registering, meaning it has to be read while in place (you can imagine how uncomfortable that would be if your wife or husband had to assist you in a rectal reading).
 Wondering about the historical accuracy of “normal,” Mackowiak set up his own experiment. He learned that a person’s temperature is “almost like a fingerprint,” unique to the individual and found the actual “normal” temperature to be 98.2 degrees. In addition, body temperature varies from one person to another. In women, it increases with ovulation and during the menstrual cycle. During vigorous exercise, temperature increases.
Wondering about the historical accuracy of “normal,” Mackowiak set up his own experiment. He learned that a person’s temperature is “almost like a fingerprint,” unique to the individual and found the actual “normal” temperature to be 98.2 degrees. In addition, body temperature varies from one person to another. In women, it increases with ovulation and during the menstrual cycle. During vigorous exercise, temperature increases.
Seattle Children’s Hospital says that many parents have “fever phobia” and in fact, fevers may be harmless and often helpful. They note that fevers turn on the body’s immune system and help the body fight infection. Read more here.
My “normal” temperature is 96.8°. What’s yours?
Blood Pressure
There are many myths associated with high blood pressure, or hypertension. The most important and insidious is that you will “feel” high blood pressure. In fact, most people with hypertension don’t have any symptoms. Unfortunately, often the first symptom is stroke, or even death.
If you do have symptoms like headache, nosebleeds or blurry vision, it can mean your hypertension has reached “severe and possibly life-threatening levels” according to Dr. Daniel Pohlman, a primary care doctor at Rush University Medical Center.
The only way to know is to get your blood pressure checked regularly. And although the risk increases with age, even children can develop hypertension, and should be checked routinely, beginning at age three.
Measuring blood pressure needs to be done correctly. According to Dr. William B. White, editor of the medical journal Blood Pressure Monitoring, blood pressure is measured incorrectly about 50% of the time.
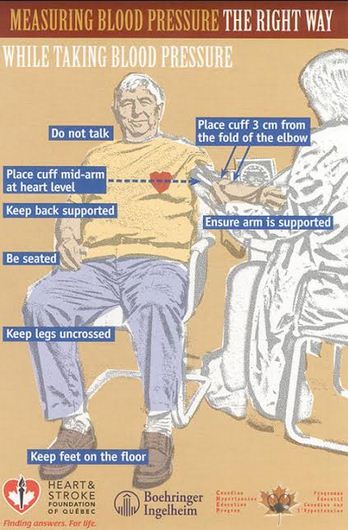
Nutrition Action lists common mistakes when measuring blood pressure:
- After consuming caffeine, which temporarily raises pressure
- Within 30 minutes of smoking — raises blood pressure
- If your bladder is full — raises pressure
- Within 30 minutes of aerobic exercise, such as jogging or even brisk walking — temporarily lowers pressure
- Sitting on a exam table or chair without back support — can raise diastolic (the lower number) pressure
- Sitting with legs dangling or crossed — raises pressure (keep your feet flat on the floor)
- With your arm above or below heart level. The person measuring your arm should be supporting your arm, not you
- Don’t speak — stay calm, because even casual conversation can raise pressure
Most importantly, before a diagnosis of hypertension or prehypertension, your blood pressure should be measured at least twice on at least two separate occasions, with good technique both times.
Two numbers represent blood pressure. The higher (systolic) number shows the pressure while the heart is beating. The lower (diastolic) numbers shows the pressure when the heart is resting between beats. According to Blood Pressure UK, ideally, we should all have a blood pressure below 120 over 80 (120/80). At this level, we have a much lower risk of heart disease or stroke. If it’s more than 120/80 and less than 140/90 they still call it “normal” but say it’s higher than ideal.
One thing that can definitely raise your blood pressure is YOU! You may be like the 20% or more of patients who have “white coat syndrome” and your blood pressure surges when measured in a clinical setting like the doctor’s office. The Harvard Health Letter reports that blood pressure changes day-to-day and hour-to-hour, even minute-to-minute, but monitoring it daily can help control it. Something about self-monitoring is helpful.
Click here for a video from MayoClinic.org demonstrating correct way to check your own blood pressure.
 And eat your fruits and vegetables. As advised in Heart.org (American Heart Association), eating potassium-rich foods helps eliminate excess sodium through the urine. Potassium helps ease tension in your blood vessel walls, which helps further lower blood pressure.
And eat your fruits and vegetables. As advised in Heart.org (American Heart Association), eating potassium-rich foods helps eliminate excess sodium through the urine. Potassium helps ease tension in your blood vessel walls, which helps further lower blood pressure.
Blood Glucose
Chronic high blood glucose is a primary risk factor for development of diabetes complications — damage to nerves (leading to painful neuropathy), to blood vessels of the retina (diabetic retinopathy), large vessel damage (cardiovascular disease), non-healing wounds (non-traumatic amputation), fungal infections, and more.
Blood glucose and blood sugar mean the same thing — the carbohydrate we eat — from fruit (fructose), milk (lactose), starches from grains and some vegetables — all are converted into glucose to provide fuel for our body. Insulin is released from the pancreas, to “unlock” the cells so the glucose can be utilized.
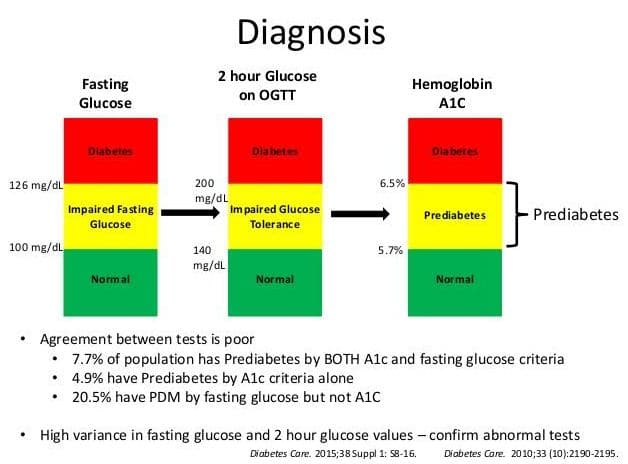
Normal blood glucose numbers will vary throughout the day depending on your meals and your activity. For someone without diabetes, a fasting blood sugar on awakening should be under 100 mg/dl. Before-meal normal sugars are 70–99 mg/dl. “Postprandial” sugars taken two hours after meals should be less than 140 mg/dl.
Hemoglobin A1C, or just ‘A1C’, is blood test that shows your average blood glucose over the previous 2-3 months.
Normal for person without diabetes: Less than 5.7%
Official American Diabetes Association recommendation for someone with diabetes: 7.0% or less.
If you are overweight or obese and you have a family history, you’re at pretty high risk for type 2 diabetes, so monitor at least yearly. Pay attention for subtle symptoms, including blurred vision, unexplained weight loss, unusual thirst, slow wound healing, or unusual fatigue.
Some blood glucose monitors are more accurate than others, but experts say that technique is typically the reason for inaccurate readings. There are a number of factors that can affect accuracy:
- Damaged or outdated test strips
- Extreme temperatures: keep meter and strips at room temperature
- Proper coding: some meters must be coded to your particular test strips
- Monitor use/functionality: make sure you’re inserting the strip properly, and that the batteries are up to snuff.
- Sample size: most monitors need a generous drop of blood to get an accurate reading.
- Red blood cell count: dehydration can skew your numbers; if you have anemia the reading is likely to be less accurate.
A good idea is to bring your monitor with you to your next doctor’s appointment or when you’re going to the lab for new tests. Check your own blood glucose level with your meter at the same time as you’re getting blood drawn for your tests. Results within 15% of the lab reading are considered accurate.
And don’t forget, most people with type 2 diabetes (about 85-90% of people with diabetes) can manage or even reverse the symptoms by getting to a healthy weight with smart eating and lots of activity, including resistance training. You can do it!
Sources
American Heart Association. How potassium can help control high blood pressure. http://www.heart.org/HEARTORG/Conditions/HighBloodPressure/MakeChangesThatMatter/How-Potassium-Can-Help-Control-High-Blood-Pressure_UCM_303243_Article.jsp#
Blood Pressure UK. What is normal blood pressure? http://www.bloodpressureuk.org/BloodPressureandyou/Thebasics/Whatisnormal
Diabetes Self-Management. What is a normal blood sugar level? http://www.diabetesselfmanagement.com/blog/what-is-a-normal-blood-sugar-level/
Freakonomics Radio on NPR. Bad Medicine, Part 1. The Story of 98.6 http://freakonomics.com/podcast/bad-medicine-part-1-story-98-6/
Harvard Health Letter. Checking blood pressure: Do try this at home. http://www.health.harvard.edu/heart-health/checking-blood-pressure-at-home
JAMA Network. A critical appraisal of 98.6°, the upper limit of the normal body temperature, and other legacies of Carl Reinhold August Wunderlich. http://jamanetwork.com/journals/jama/article-abstract/400116
MayoClinic.org. Diabetes. Sometimes my blood glucose monitor seems to give incorrect readings. What can I do to make sure the measurement is accurate? http://www.mayoclinic.org/diseases-conditions/diabetes/expert-answers/blood-glucose-monitors/faq-20057902
MayoClinic.org. Video: How to measure blood pressure using an automatic monitor. https://www.mayoclinic.org/diseases-conditions/high-blood-pressure/multimedia/how-to-measure-blood-pressure/vid-20084749
Nutrition Action. Don’t let your doctor make these 9 blood pressure measurement mistakes. http://www.nutritionaction.com/daily/heart-and-disease-cat/dont-let-your-doctor-make-these-9-blood-pressure-measurement-mistakes/
QJM: An International Journal of Medicine. A brief history of the clinical thermometer. https://academic.oup.com/qjmed/article/95/4/251/1562440
Rush University Medical Center. Myths about high blood pressure. https://www.rush.edu/health-wellness/discover-health/high-blood-pressure-myths
Seattle Children’s Hospital. Fever — Myths Versus Facts. http://www.seattlechildrens.org/medical-conditions/symptom-index/fever-myths-versus-facts/
University of Michigan Health System. Body Temperature. http://www.uofmhealth.org/health-library/hw198785

















