Coronavirus: Why is it called ‘novel’ and should you wear a face mask? What about your pet?
By Nicoletta Lanese
Coronaviruses make up a large family of viruses that can infect birds and mammals, including humans, according to the World Health Organization (WHO). 
These viruses have been responsible for several outbreaks around the world, including the severe acute respiratory syndrome (SARS) pandemic of 2002-2003 and the Middle East respiratory syndrome (MERS) outbreak in South Korea in 2015. Most recently, a novel coronavirus (2019-nCoV) triggered an outbreak in China in December 2019, sparking international concern.
While some coronaviruses have caused devastating epidemics, others cause mild to moderate respiratory infections, like the common cold.
Causes
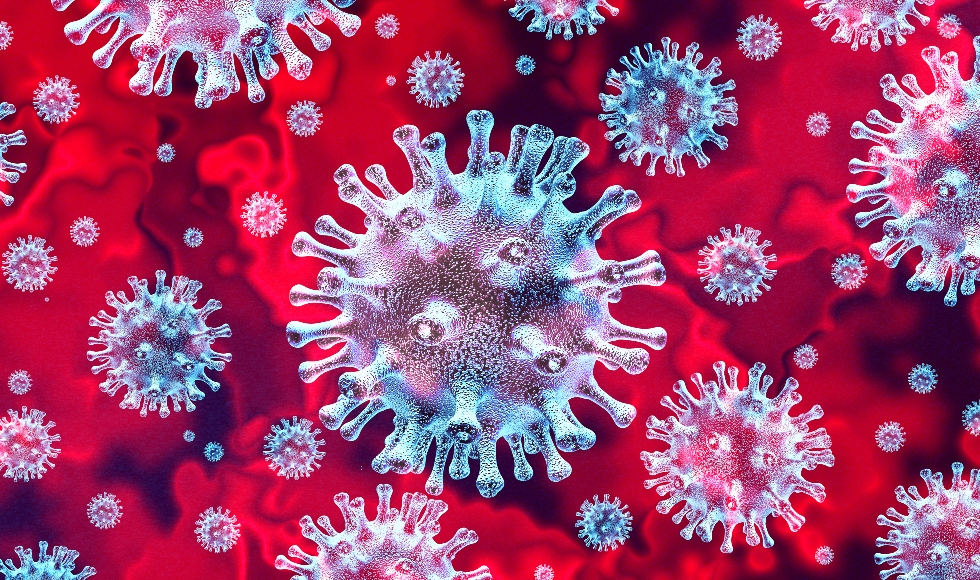 All coronaviruses sport spiky projections on their outer surfaces that resemble the points of a crown, or “corona” in Latin, according to the Centers for Disease Control and Prevention (CDC). Seven known coronaviruses can infect humans, including the novel coronavirus identified in 2019.
All coronaviruses sport spiky projections on their outer surfaces that resemble the points of a crown, or “corona” in Latin, according to the Centers for Disease Control and Prevention (CDC). Seven known coronaviruses can infect humans, including the novel coronavirus identified in 2019.
Beneath a coronavirus’s pronged exterior lies a round core shrouded in proteins and a “greasy” membrane, Jan Carette, an associate professor of microbiology and immunology at the Stanford University School of Medicine, told Live Science in an email. The core contains genetic material that the virus can inject into vulnerable cells to infect them. So-called spike proteins extend from within the core to the viral surface and allow the virus to “recognize and latch onto” specific cells in the body, Carette said.
“When the spike engages its receptor [on a host cell], a cascade is triggered, resulting in the merger of the virus with the cell,” he added. This merger allows the virus to release its genetic material and hijack the cell’s internal machinery. “Once this happens, the virus sheds its coat and turns the cell into a factory that starts churning out new viruses.”
Several coronaviruses utilize animals as their primary hosts and have evolved to infect humans, too. Precursors to both SARS and MERS coronaviruses appear in bats. The SARS virus jumped from bats to civets (small, nocturnal mammals) on its way into people, while MERS infected camels before spreading to humans. Evidence suggests that the novel coronavirus also jumped from bats to humans after passing through an intermediate carrier, although scientists have not yet identified the infectious middleman creature.
The four most common human coronaviruses — named 229E, NL63, OC43 and HKU1 — did not jump from animals to humans but rather utilize humans as their natural hosts, according to the CDC. These human-borne coronaviruses “have presumably evolved to maximize spread amongst the population rather than pathogenicity,” meaning the viruses may opt to maximize their spread rather than harm their human host, Carette said. This may explain why coronaviruses that are transmitted from animals seem to cause more-severe diseases in humans, but the idea remains speculative, he added.
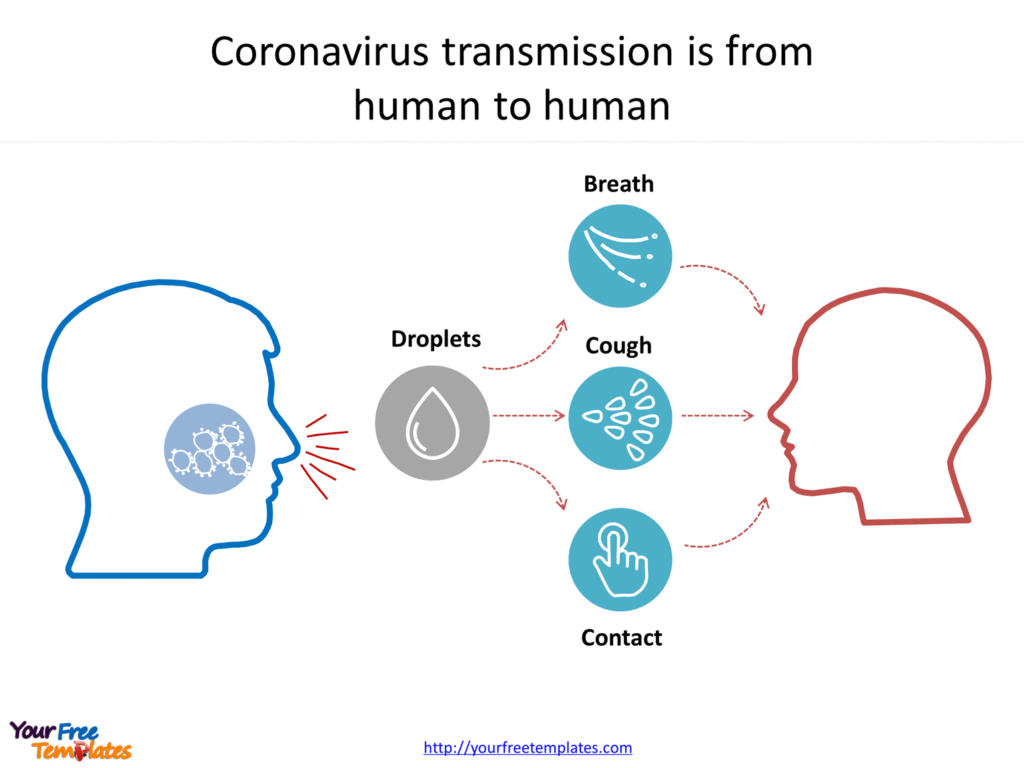 Coronaviruses can be transmitted between humans through respiratory droplets that infected people expel when they breathe, cough or sneeze. A typical surgical mask cannot block out the viral particles contained in these droplets, but simple measures — such as washing your hands, disinfecting frequently touched surfaces and objects, and avoiding touching your face, eyes and mouth — can greatly lower your risk of infection.
Coronaviruses can be transmitted between humans through respiratory droplets that infected people expel when they breathe, cough or sneeze. A typical surgical mask cannot block out the viral particles contained in these droplets, but simple measures — such as washing your hands, disinfecting frequently touched surfaces and objects, and avoiding touching your face, eyes and mouth — can greatly lower your risk of infection.
The viruses generally cannot survive for more than a few hours on surfaces outside a human host, but people can pick up a coronavirus from a contaminated surface for a short window of time, Dr. Nancy Messonnier, director of the Center for the National Center for Immunization and Respiratory Diseases, said during a CDC news conference in early 2019. Scientists don’t yet know how long the novel coronavirus can survive outside a host.
Symptoms
In humans, coronaviruses typically cause a respiratory infection with mild to severe flu-like symptoms, but the exact symptoms vary depending on the type of coronavirus.
The four common human coronaviruses can cause people to develop a runny nose, headache, cough, sore throat and fever, according to the CDC. In a subset of individuals, including those with cardiopulmonary disease or a weakened immune system, the viral infection can progress to a more severe lower-respiratory infection such as pneumonia or bronchitis.
In comparison, severe MERS and SARS infections often progress to pneumonia. Other symptoms of MERS include fever, coughing and shortness of breath, while SARS can cause fever, chills and body aches. SARS had a mortality rate of 9.6% in the early 2000s outbreaks, according to The New York Times, while MERS has an estimated mortality rate between 30% and 40%, the CDC noted.
The novel coronavirus causes symptoms similar to those of other coronaviruses, triggering fever, cough and difficulty breathing in most patients. Rarer symptoms include dizziness, nausea, vomiting and a runny nose. As of February 2019, scientists estimate the 2019-nCoV mortality rate at 2%, although that figure may be somewhat skewed by the severity of the cases studied so far. As more mild cases of the infection are accounted for, the estimated mortality rate may fall.
Doctors can test their patients for coronavirus infections by analyzing respiratory specimens and serum isolated from their blood, according to the CDC. The CDC has developed an equivalent diagnostic test for the novel coronavirus, but its accuracy and specificity for the virus are still being verified. Once confirmed, diagnostic kits will be distributed to health care facilities in the U.S. and abroad, according to a CDC news conference in January 2019.
 There are no available treatments for any human coronavirus, according to the CDC. Those who catch a common coronavirus usually recover on their own and can ease the process by taking pain and fever medications, using a humidifier, taking hot showers, drinking plenty of fluids and staying home to rest. Similar regimens are used to relieve the symptoms of more severe coronavirus infections.
There are no available treatments for any human coronavirus, according to the CDC. Those who catch a common coronavirus usually recover on their own and can ease the process by taking pain and fever medications, using a humidifier, taking hot showers, drinking plenty of fluids and staying home to rest. Similar regimens are used to relieve the symptoms of more severe coronavirus infections.
Several existing antiviral medications, originally intended to treat Ebola and malaria, may show some efficacy against the novel coronavirus, Live Science previously reported. These medications disable viruses by interfering with their attempts to replicate in host cells. Another class of drug, called “protease inhibitors,” also shows promise against coronaviruses and helps to alert the immune system to viral invaders.
As of February 2019, no federally approved vaccines exist to prevent coronavirus infections.
Scientists developed a candidate vaccine for SARS during the pandemic of that virus, and a potential MERS vaccine recently performed well in preliminary clinical trials, but neither of these has hit the market. Research groups around the world are now racing to develop a vaccine for the novel coronavirus; the CDC aims to have such a vaccine ready for clinical trials within three months. If and when a vaccine is developed, however, health officials will have to evaluate how the outbreak has evolved before conducting further tests and eventually administering the vaccine.
Can wearing a medical face mask protect you against the new coronavirus? It’s a question many people, including pet owners who are putting canine face masks on their dogs, are asking.
If it’s a regular surgical face mask, the answer is “no,” Dr. William Schaffner, an infectious-disease specialist at Vanderbilt University in Tennessee, told Live Science.
A more specialized mask, known as an N95 respirator, can protect against the new coronavirus, also called 2019-nCoV. The respirator is thicker than a surgical mask, but Schaffner doesn’t recommend it for public use, at least not at this point.

Despite the fact that the World Health Organization (WHO) reported that there is no evidence suggesting house animals can be infected with the new strain of coronavirus, Chinese people have still gone one step further to protect their pets from a potential threat. Sales of pet masks have reportedly skyrocketed since the initial outbreak of the coronavirus and don’t seem to be stopping anytime soon.
Additional resources:
- Review these FAQs about the novel coronavirus from the CDC.
- Learn more about coronaviruses from the World Health Organization.
- Read about 10 deadly diseases that hopped across species.
- Read Can wearing a facemask protect you from the new coronavirus?
This article is for informational purposes only, and is not meant to provide medical advice.
______________________________
Credit: LiveScience.com.























