What should your poop look like?
Drug advertisements. Ugh. By the time they finish listing the side effects, you wonder why they even bother publicizing them? Have you noticed that almost every advertisement on the U.S. news show ’60 Minutes’ is for some pharmaceutical drug, or more recently, for a test to detect colon cancer? But this ad doesn’t sound so bad. Testing for colon cancer without all of the dreaded prep?
pharmaceutical drug, or more recently, for a test to detect colon cancer? But this ad doesn’t sound so bad. Testing for colon cancer without all of the dreaded prep?
According to media researcher Quartz, ‘Big Pharma’ spent almost about $27 billion on marketing for prescription drugs and any health conditions that may be associated with them — earning a hefty return for the companies, about $329 billion.
As announced in August of 2018, the world’s largest pharmaceutical company, Pfizer Inc., has joined with Exact Sciences Corp to market Cologuard, committing to spending $138 million on marketing through 2021.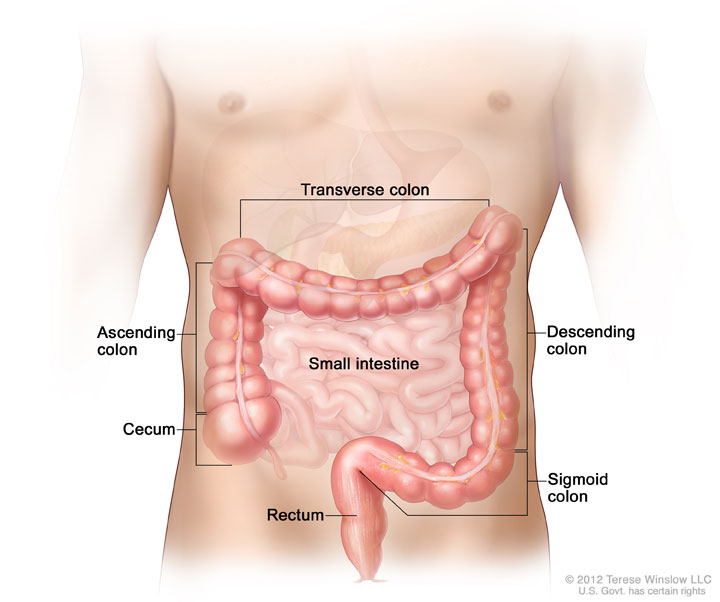
Cologuard is a non-invasive screening test for colorectal cancer. Available by prescription only, the company sends you a boxed kit, including a poop collector and preservative, and you produce a sample to send back to the company’s lab. The test identifies the presence of red blood cells and DNA mutations that may be cancers such as colon cancer or precursors to cancer.
Anyone who has had a colonoscopy can attest to the attractiveness of the advertisements. Some of the print phrases are downright reassuring. “Do-it-yourself”, “screening made easy”, “convenient” and “non-invasive”. On YouTube, I watched some of the televised ads. In one, a nice lady in the window says, “I’m not doing that! I eat plenty of kale!” Another says, “All that prep? No thanks! That drink tastes horrible.”

But is Cologuard as effective as a colonoscopy?
Well… it should tell you something when the tiny white print appears on the screen that says, “Any positive should be followed by a diagnostic colonoscopy.”
Yes, a colonoscopy requires prep. For sure. Your colon has to be empty and clean so the doctor can properly image the entire colon. You need to fast and take laxatives and drink liquids — lots and lots of liquids prior to the test. So this new “easy” test sounds attractive.
The colon is the lower portion of the GI tract and where nutrients are absorbed and waste is created. During a colonoscopy, the doctor uses a thin, flexible camera to look for abnormalities including signs of cancer. However, a colonoscopy is performed as both a screening procedure and a possible treatment procedure. A colonoscopy is considered positive if the doctor finds any polyps or abnormal tissue in the colon. Most polyps aren’t cancerous, but some can be pre-cancerous. Polyps removed during colonoscopy are sent to a laboratory for analysis to determine whether they are cancerous, precancerous or noncancerous.
The Digestive Diseases Center writes that colonoscopies can detect 95 percent of all colorectal cancers and advanced precancerous polyps.
To date, studies have shown that Cologuard detects 92 percent of colorectal cancers but only 42 percent of precancerous polyps.
A colonoscopy will provide a definitive diagnosis — the doctor will be able to say, hey, you’re good, no polyps, see you in 10 years (if you have no risk factors and no polyps), but even if you get a negative result from the Cologuard test, the recommendation is to repeat the test in three years. There is also a 13 percent false positive rate for this non-visual test. Which would mean you need a follow-up colonoscopy.
If you have health insurance, the Cologuard test may be covered. If not, it’s $649, and they recommend the test be repeated every three years.
Oh. And if you have a positive result from the Cologuard test, you’ll have to have a colonoscopy anyway, to confirm the results.
Colorectal cancer (CRC) is the second-leading cause of cancer deaths in the USA, after lung cancer — more than 50,000 Americans die from colon cancer yearly. CRC was among the five most common cancers diagnosed in Central and South America, and in Ecuador, more women than men die from it.
According to the Pan American Health Organization (PAHO) age, family history, race or ethnic background are among the main non-modifiable risk factors for CRC, but diet, physical activity, weight, smoking, and alcohol consumption are risk factors that you can control and reduce your risk for cancer.
There are two types of fecal occult blood tests: the guaiac-based FOBT is provided by the doctor’s office or a lab and done at home. The stool sample is placed on a test card and if it changes color it means there is blood in the stool and you need further testing…like…a colonoscopy.
The fecal immunochemical test (FIT) screens for hidden blood in the stool, which can be an early sign of cancer, but it’s not a diagnostic test and only detects blood from the lower intestine. If it comes out positive, the doctor will want to perform additional tests, including… a colonoscopy.
As the PAHO reports, screening for CRC can effectively reduce mortality but costs are a huge barrier to population screenings. They cite a Colombian study that compared six different screening strategies and concluded that only one of them (FOBT every two years) was cost-effective for the country.
 If precancerous polyps are found early, colon cancer is one of the most preventable cancers because during a colonoscopy any polyps will typically be removed.
If precancerous polyps are found early, colon cancer is one of the most preventable cancers because during a colonoscopy any polyps will typically be removed.
“Don’t Assume” is the Colorectal Cancer Alliance’s 2019 National Colorectal Cancer Awareness Month public awareness campaign.
The four assumptions are:
1. Don’t assume you’re too young for colorectal cancer
2. Don’t assume you’re alone
3. Don’t assume we can’t beat colorectal cancer
4. Don’t assume you can’t save your own ass! [I love this!]
From the National Cancer Institute:
Colorectal Cancer Screening
- Tests are used to screen for different types of cancer.
- Studies show that some screening tests for colorectal cancer help find cancer at an early stage and may decrease the number of deaths from the disease.
- Five types of tests are used to screen for colorectal cancer:
- Fecal occult blood test
- Sigmoidoscopy
- Colonoscopy
- Virtual colonoscopy
- DNA stool test
- Studies have shown that screening for colorectal cancer using digital rectal exam does not decrease the number of deaths from the disease.
The “virtual colonoscopy” uses X-ray technology to inspect the colon. Benjamin Lebwohl, MD, a gastroenterologist at Columbia Doctors Eastside in New York City suggests, “ This is a promising technology, but is probably less effective than colonoscopy at detecting small polyps.”
And as with the other non-invasive tests, a positive result means you’ll need to have a colonoscopy.
There’s a pattern here.
Naresh Gunaratnam, M.D., a gastroenterologist and research director at Huron Gastroenterology in Ypsilanti, Michigan writes, “Preventing cancer is even better than finding it early. If our goal is to prevent colorectal cancer, then finding, quantifying, localizing, and removing polyps is the most effective strategy.” He notes that individuals on Medicare who opt for the Cologuard test and receive a positive test may be faced with out-of-pocket bills. Insurance will cover 100 percent of the cost of colonoscopy as a preventative screening test, but a follow-up colonoscopy for a positive Cologuard is considered a diagnostic or therapeutic service and may not be covered.
By the way, I called the company, and Cologuard is not available in Ecuador.
Prevention
See your doctor if you experience any of the following symptoms for more than a few days:
- Bright red, black, or very dark blood in your stool
- A change in bowel movements, including a change in the shape of the stool. Watch this fun (I’m not kidding!) and informative video and learn what to looks healthy and what does not. Click here.
- Discomfort when having a BM
- Cramping in your lower abdomen
- Frequent gas pains
- Losing weight without trying
- Constant fatigue.

Some think it’s funny. Others don’t want to talk about it. But one way or another, everyone has to poop, and the state of your bowel movements can actually be pretty telling of your overall health. Credit: Health Freedom Alliance
Do you think you’re too young to get screened? The CCA says, “your ass may look great, but if you’re having symptoms talk to your doctor about getting screened.”
The American Cancer Society (ACS) has released an updated guideline for colorectal cancer screening. Among the major guideline changes, the new recommendations say screening should begin at age 45 for people at average risk. Previously, the guideline-recommended screening begins at age 50 for people at average risk. Recommendations for screening test options are also part of the guideline changes.
Those with a first-degree relative (mom, dad, sister, brother) who had colon cancer at age 60 or younger should start at age 40 or 10 years before the age that their family member was diagnosed.
People who are in good health and with a life expectancy of more than 10 years should continue regular colorectal cancer screening through the age of 75.
People ages 76 through 85 should make a decision with their medical provider about whether to be screened, based on their own personal preferences, life expectancy, overall health, and prior screening history.
People over 85 should no longer get colorectal cancer screening.
Learn more about preparing for a colonoscopy for Harvard Health here. It is not so bad, and I bet you know someone whose life was saved by having a colonoscopy.
The Takeaway: Cologuard Testing vs. Colonoscopy
Credit Brian K. Cooley, MD
Cologuard:
Combines:
• DNA testing for mutations (KRAS, NDRG4, BMP3, B-Actin)
• Fecal Immunoglobulin Test (FIT) for globulin
• Not indicated for high risk (family history of colon cancer, personal history of colon polyps, IBD) or symptomatic patients
Cologuard Pros:
• Non-invasive
• No bowel prep
• Covered by Medicare
• Convenient
Cologuard Cons:
• Misses 8% of colorectal cancer
• Misses 60% of advanced polyps
• Cost: Checking online, the list price of Cologuard is $649. Insurance may cover some or all of that amount depending on the patient’s insurance plan and benefits – vs FIT $22 (Medicare). I checked Amazon.com, and there are a myriad of occult blood home tests available.
• 13% false positive rate, increases with age
• Required every 3 years, may result in patient non-compliance
• Considered a 2nd Tier test, offer only if Colonoscopy or annual FIT is refused*
Colonoscopy Pros:
• Gold standard for detection of all cancerous and precancerous lesions
• Best test for prevention of colorectal cancer and related deaths
• Covered by Medicare and less expensive than Cologuard every 3 years
• Every 10 years in average-risk patients
• Only acceptable test in symptomatic patients (e.g. Iron deficiency anemia, bleeding, change in bowel habits)
• Preferred first tier according to the multi-society task force on colon cancer**
Colonoscopy Cons:
• Invasive
• Requires bowel prep
• Operator dependent
• Sedated procedure
• Very small risk of complication
When Should I Be Screened for Colon Cancer?
Colon cancer can occur without any signs or symptoms. For this reason, Dr. Cooley recommends following the recommended American College of Gastroenterology screening guidelines:
• If you don’t have a family history of colon cancer, the new American Cancer Society guidelines recommend your first colonoscopy at age 45.
• There is some recent evidence that African Americans are at higher risk of developing colon cancer at a younger age and therefore should start colon cancer screening at age 45.
• If one or more first-degree relative(parent, sibling or child) has had a precancerous polyp or colon cancer, you should have your first colon examination 10 years younger than the youngest age of the family member with colon cancer, or age 40, whichever is younger.z
• There are other guidelines for specific disease states like ulcerative colitis or Crohn’s disease that should be discussed with your doctor. Also, certain familial cancer syndrome patients need to be screened at a much younger age.
Here’s a fun video of a consumer’s reaction to Cologuard instructions.
Sources
American Cancer Society. American Cancer Society Updates Colorectal Cancer Screening Guideline.
Colorectal Cancer Alliance. March is National Colorectal Cancer Awareness Month
EverydayHealth.com. What you can do to prevent colon cancer.
National Cancer Institute. Tests to Detect Colorectal Cancer and Polyps.
Pan American Health Organization. Colorectal Cancer Screening in the Americas: Situation and Challenges.
STATNews.com. Colorectal cancer screening: Science should trump convenience.
Food, Nutrition, and Your Health columnist Susan Burke March moved to Cuenca after 35 years as a Registered and Licensed Dietitian and Certified Diabetes Educator in the United States. She currently serves as the Country Representative from Ecuador for the Academy of Nutrition and Dietetics.
Susan helps people attain better weight and health, and reduce the risk of heart disease, diabetes, and other conditions that can be improved with smart lifestyle modifications. Contact her at SusantheDietitian@gmail.com.
























