Some common medicines may increase the risk for dementia
By Pam Belluck
Can certain medications increase your risk of dementia?
A new study suggests that people who take a class of common medicines called anticholinergic drugs for several years may be more likely to develop dementia as they age.
This is not a new hypothesis about these drugs, which are used to treat a wide range of conditions from depression to epilepsy to incontinence. But the study, published in the journal JAMA Internal Medicine, is large, and it analyzed the use of the medications in more detail and over a longer period of time than many previous studies.
Here’s what is known about the potential link between anticholinergic medicines and dementia:
Which drugs are we talking about?
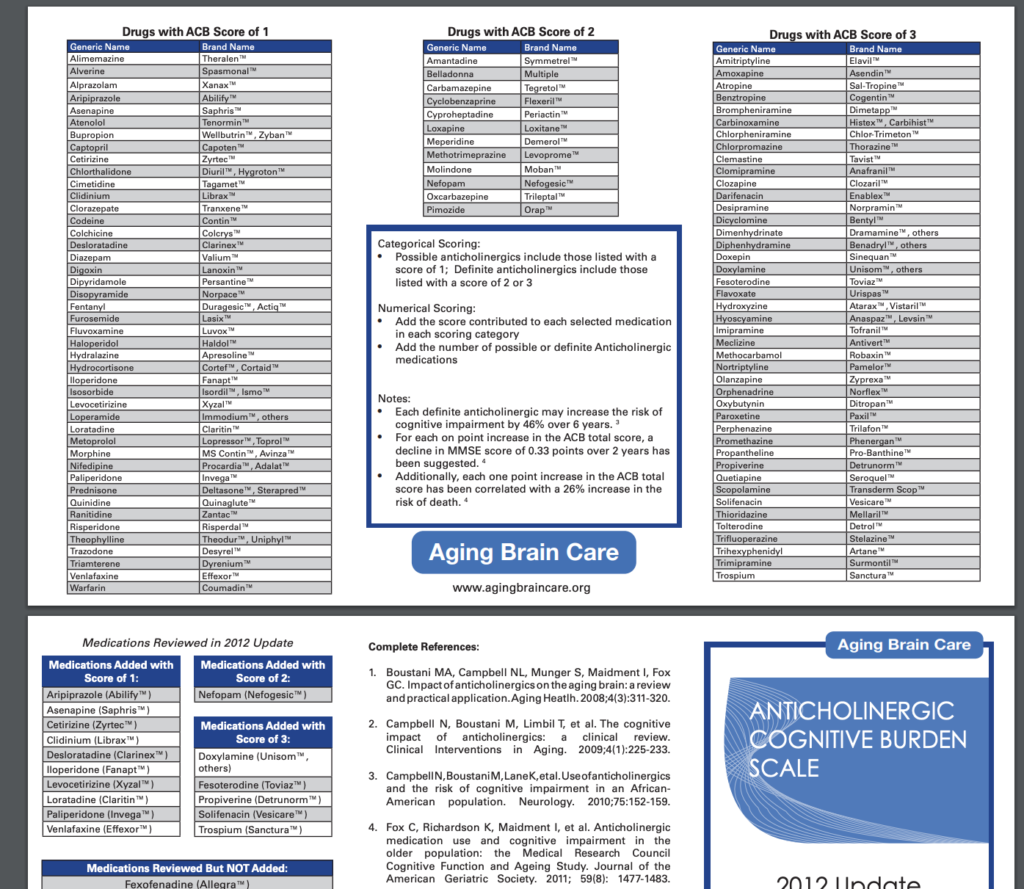
Anticholinergic drugs include the antipsychotic clozapine; the bladder drug darifenacin (marketed as Enablex); the anti-nausea drug scopolamine; the bronchodilator ipratropium; the muscle relaxant tizanidine; antihistamines such as diphenhydramine (brand names include Benadryl), and antidepressants such as paroxetine (brand names include Paxil).
These medications work by blocking a chemical called acetylcholine, which acts as a neurotransmitter and is involved in many nervous system functions including muscle movements, heart rate, the widening of blood vessels, respiratory functions and muscle contractions in the stomach during digestion.
Older adults are more likely to be prescribed many of these medications, simply because they tend to have more health issues. Some experts say that because people produce less acetylcholine as they age, drugs that inhibit that neurochemical can have a stronger effect on older people.
 What does previous research show?
What does previous research show?
Other studies have also suggested that long-term use of some anticholinergic medications might increase the risk that older people will develop dementia.
For example, a 2015 study by researchers at the University of Washington found that people age 65 and older who took these medications for three years or more had a 54 percent greater risk of developing dementia than people who took the medications for three months or less.
A 2014 review found more than 30 studies that suggested confusion and other symptoms of cognitive decline increase with the amount of anticholinergic medication someone takes.
Dr. Malaz Boustani, director of the Regenstrief Center for Health Innovation and Implementation Science at Indiana University, has created a tool called the anticholinergic cognitive burden scale, which ranks drugs by their suspected effects on cognition. Experts suggest avoiding extended use of drugs with a rating of 3 on the scale — or combinations of drugs that together rate 3 or higher.
What did the new study involve?
The research, conducted by Carol Coupland, a professor of medical statistics in primary care at the University of Nottingham in England, and colleagues, evaluated anticholinergic drugs prescribed to nearly 285,000 people age 55 and older. About 59,000 of them had a diagnosis of dementia. The information came from a database of medical records from patients in more than 1,500 general practices in Britain, the authors said.
Researchers looked at the medical records of patients who were diagnosed with dementia and examined the drugs they had been prescribed from 11 years to one year before their diagnosis. They compared their medications during that time frame with those of people who did not have a diagnosis of dementia. They recorded which of 56 anticholinergic medications people were prescribed, and at what dose and how long. They accounted for factors like body mass index, smoking, alcohol consumption, other medical conditions and use of other medications.
The study found a 50 percent increased risk of dementia among people who used a strong anticholinergic drug daily for about three years within that 10-year period. The association was stronger for antidepressants, bladder drugs, antipsychotics and epilepsy medications, the study said. Researchers did not find any increased risk of dementia with antihistamines, bronchodilators, muscle relaxants or medications for stomach spasms or heart arrhythmias.
The link between anticholinergic drugs was stronger for people diagnosed with dementia before they turned 80 and in people with vascular dementia compared to people with Alzheimer’s disease, the authors reported.

What are the limitations of the research?
An important caveat with this type of study is that it is observational — meaning there is no way to know if the medication use played any direct role in causing dementia. All it shows is that the risk of developing dementia appears to be higher for people who take some of these medications.
It’s also possible, the authors note, some conditions, like depression, may be early harbingers of cognitive decline. It’s possible, for example, that some people taking antidepressants might actually be being treated for what will turn out to be an early symptom of dementia, so it’s their depression that goes along with an increased risk of dementia — not the medicine they are taking to treat it.
What’s the bottom line?
It’s possible, but not proven, that some anticholinergic drugs increase the risk of dementia. If you need long-term treatment for one of the relevant medical conditions, talk to your doctor about other medication options that are not in the anticholinergic class, such as antidepressants like Celexa and Prozac. In many cases, there may be choices.
Editor’s Note: Read the full study in JAMA Internal Medicine here.
_________________________________
Credit: The New York Times