With public health in crisis, Ecuador must make big changes to accommodate an aging population
By Lance Martínez
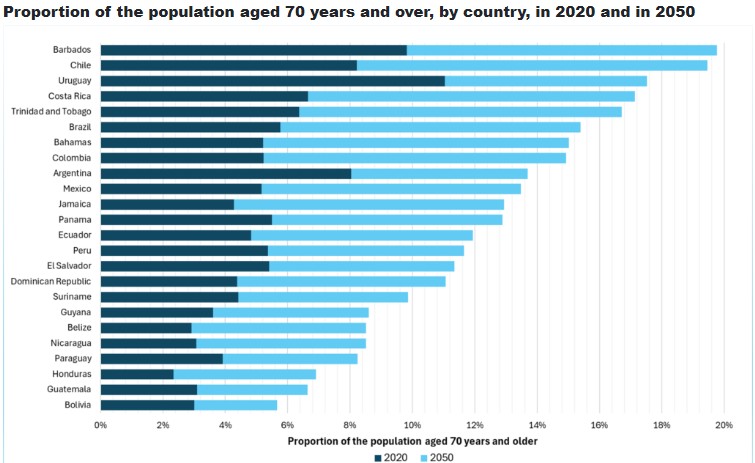
Like other Latin American countries, Ecuador faces a public health dilemma. While everyone agrees that spending on public health is woefully inadequate, the proportion of the population over the age of 70 is expected to triple within 25 years.

The aging population in Ecuador will require greater public health spending as well as more specialized services.
The current annual per capita allocation for public health is $485 – about average for Latin American and Caribbean countries — the Inter-American Development Bank (IDB) predicts spending will need to increase to $1,500 by 2050 based on increasing needs of the elderly.
“We are already in a crisis situation with our public health and Social Security systems,” says Oscar Iglesias, a health strategies professor at San Francisco University in Quito. “Patients are waiting four to five months to see medical specialists and the IESS and public health service can’t afford to buy needed medications.”
Iglesias adds that the crisis affects the entire region. “Chile and Uruguay have the best-funded public health in South America, spending about $800 per person annually, but they also have long waits for medical appointments and a shortage of medicine.”
The recent IDB report says the amount spent on public health is not the only problem. “Better planning and smarter spending would optimize current expenditures,” it says. Countries that apply cost-effectiveness criteria, data-driven planning, and strategic negotiation with drug suppliers achieve better results with less money. This is more important than ever as the elderly population increases.”
To meet the needs of older adults, the IDB says, investment in treatment for the elderly “must increase dramatically”, especially in the areas of cancer, diabetes or cardiovascular diseases.
Iglesias, who participated in the IDB study, says the final report offers a “roadmap” to smarter health care spending but also emphasizes the need for a substantial increase in spending.
The report offers five “keys to smart public health spending” in Ecuador. (Article continues below graphic)
1) Invest in primary care and prevention
Ecuador allocates a minimal part of its budget to prevention and health promotion. On the other hand, the bulk goes to hospitals and highly specialized services. This is more costly and inefficient. Investing more in primary care would make it possible to detect chronic diseases such as hypertension or diabetes in early stages, avoiding costly complications such as kidney failure and heart attacks.
In Azuay Province, a telehealth pilot project implemented during the pandemic made it possible to provide basic care to rural communities that previously did not have access to regular check-ups. The cost was 60% lower than face-to-face visits and improved treatments in older adults.
2) Reform the way medicines and services are purchased
In Ecuador, procurement processes are still mostly manual, slow and uncompetitive. This generates high prices, shortages and corruption. According to the IDB, bureaucratic processes discourage the participation of suppliers and raise transaction costs. Many drugs are still bought by inertia, without reviewing their effectiveness or relevance.
The recommendation is to digitize and centralize purchases, as Chile already does (through Cenabast, which has generated savings of up to 75%). Ecuador could move towards a national procurement agency that negotiates prices at scale and avoids duplication in bidding processes.
3) Eliminate inefficient spending
The IDB study indicates that up to one-third of health spending may be clinically unnecessary or ineffective. This includes duplicate prescriptions, avoidable hospitalizations, unnecessary testing, and improper medications. Ecuador, with a fragmented system between the Ministry of Public Health, the IESS, the Armed Forces and the Police, multiplies the risk of this waste. Procurement should be centralized among the systems.
The lack of interoperability between medical record systems leads to repeated examinations every time a patient changes networks. Implementing a single national medical record would save millions in duplicate tests.
4) Strengthen institutionality and accountability
Lack of transparency in hospital administration and in public insurance such as the IESS has caused loss of resources, corruption and lack of transparency. The IDB recommends implementing explicit benefit plans (PBS), which clearly inform which services are covered, and facilitate evaluation of results and accountability.
Ecuador does not yet have a consolidated PBS at the national level. Implementing it would guarantee basic basket of services, monitoring its compliance and evaluating the impact on health in a systematic way.
5) Reduce the financial burden on households
In Ecuador, out-of-pocket health care spending averages more than 40% of total health spending, well above the WHO recommended average of 15%. This means that many people must pay directly for consultations, medications or treatments, which leads to indebtedness or failure to receive critical treatment.
“Public investment must be strengthened, the fragmentation of the system must be reduced and the different actors must be coordinated to guarantee universal coverage,” the IDB report says. “In practice, this would imply, for example, expanding free access to essential medicines, incorporating cost-effectiveness criteria in the selection of drugs and unifying financial information systems.”